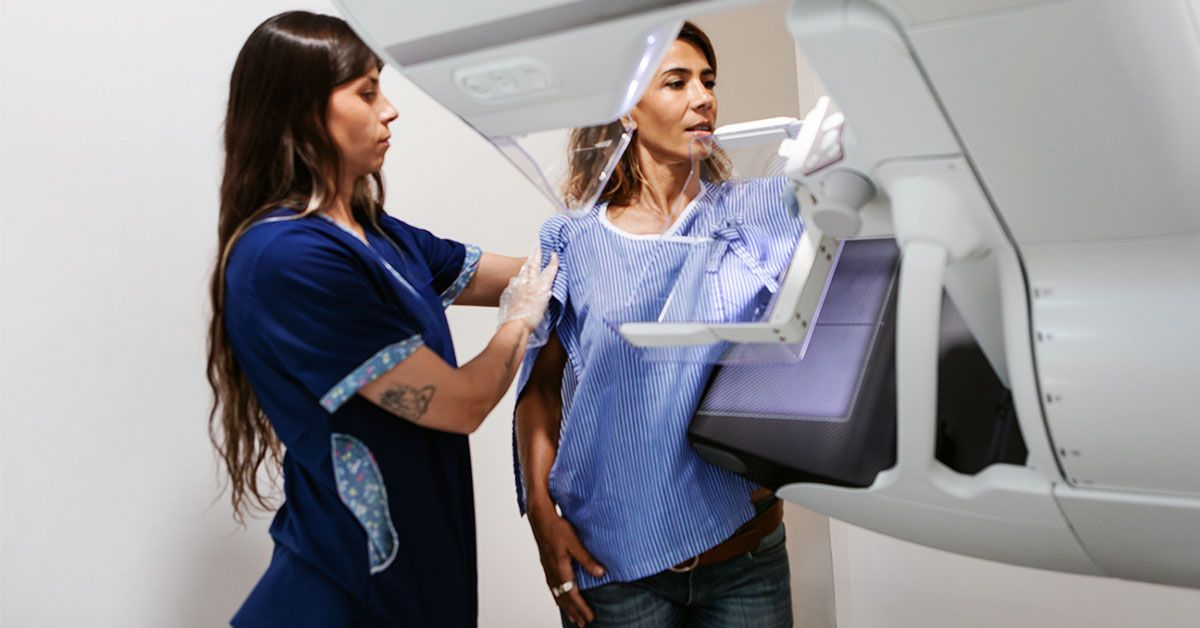
- New guidance from the American College of Physicians (ACP) recommends biennial mammography for average-risk females aged 50 to 74 to screen for breast cancer.
- For those aged 40 to 49, the ACP advises that screening should be individualized through shared decision-making, considering personal risk and potential harms like false positives and overdiagnosis.
- They also suggest routine screening is not generally recommended after age 74, especially for those with limited life expectancy, due to uncertain benefits and increased risks.
- For individuals with dense breasts, 3D mammography may be considered, but additional imaging is not routinely advised for those at average risk.
Breast cancer is one of the most common cancers in American women, accounting for
Breast cancer mainly occurs in middle-aged and older women, with most breast cancers found in females who are
Breast cancer screening plays a
A new guidance statement from the ACP, presented at the ACP’s 2026 Internal Medicine Meeting and published in the Annals of Internal Medicine, updates previous recommendations and adds further clarity on when to begin and stop screening.
The new guidance from the ACP advises that all asymptomatic females at average risk of breast cancer should receive mammography screening every 2 years between the ages of 50 and 74.
The guidance defines average-risk women as those who do not have a personal or family history of breast cancer, any known high risk gene variations, such as BRCA1 or BRCA 2, or prior high-dose chest radiation at a young age.
Using high-quality clinical guidelines from national guideline developers around the world, the organization concludes that this cohort is at the highest risk for developing breast cancer and most likely to receive the most benefit from mammography screening.
Amir Qaseem, MD, PhD, MHA, MGIN, FRCP, FACP, Senior Vice President of Clinical Policy and the Center for Evidence Reviews at the American College of Physicians (ACP), and first author of the new guidelines, spoke to Medical News Today about the key factors behind the biennial recommendation.
“Annual screening resulted in more false-positive recalls and biopsies than biennial screening. Annual screening creates additional patient burden and costs and current evidence does not show added benefit of annual screening over biennial screening,” he said.
“Therefore, the ACP says clinicians should initiate biennial mammography in asymptomatic, average-risk females aged 50 to 74 years.”
— Amir Qaseem, MD, PhD
Additionally, while other guidance may suggest breast cancer screening every other year starting at age 40, the ACP advises those between 40 and 49 to discuss the benefits and harms of screening with their doctor.
“For asymptomatic, average-risk females aged 40 to 49 years, clinicians should use shared decision making. It’s a personal choice. Clinicians should discuss the individual patient’s risk for breast cancer, her values and preferences, and uncertainty around the benefits and harms of screening for breast cancer,” Qaseem told MNT.
“There is a small absolute reduction in mortality (only in ages 45 to 49 years) but no difference in advanced breast cancers, which needs to be balanced against harms,” he said.
“These include overdiagnosis, overtreatment, false-negative findings, increased risk of additional tests, false positive-related psychological distress, additional radiation exposure, and false positive results can reduce adherence to future screening,” he further explained.
Other guidance from the ACP also addresses screening in older populations. For women aged 75 years and older, or those with limited life expectancy, the organization recommends discussing whether to discontinue routine screening.
“Clinicians should discuss discontinuation of breast cancer screening based on shared decision making in asymptomatic average risk females aged 75 years or older or with a limited life expectancy,” Qaseem said to MNT.
“Continuing screening beyond the age of 74 showed no difference in breast cancer mortality but resulted in additional testing with or without biopsy and overdiagnoses.”
Additionally, other guidance suggests that clinicians may consider using supplemental digital breast tomosynthesis (DBT) for females with dense breast tissue.
“Clinicians should consider using supplemental DBT in females with breast density of BI-RADS category C or D based on benefits, harms, additional radiation exposure, availability, values and preferences, and costs. However, do not use supplemental MRI or ultrasound in females with breast density of BI RADS C or D,” Qaseem told MNT.
DBT describes a 3D mammography technique that may be
The ACP note their updated statement aims to help patients navigate complex trade-offs around screening frequency, age thresholds, and imaging options, and help guide clinicians on screening for breast cancer in asymptomatic, average-risk adult females.
The organization emphasizes that screening decisions should be guided by the best available evidence and tailored to individual patients.
However, health experts have voiced concerns that the ACP’s guidance relies on outdated data and risks increased mortality.
Debra Patt, MD, PhD, MBA, Executive Vice President of Public Policy and Strategy for Texas Oncology, told MNT her views on the updated guidance.
“We are concerned that the ACP guidelines will lead to delayed diagnoses, particularly among young women 40 to 49 and women with dense breasts. The American College of Radiology and the Society for Breast Imaging have both voiced concerns about the diminished screening recommendations.”
— Debra Patt, MD, PhD, MBA
“To be clear, annual mammography in women 40 to 49 who are average risk leads to earlier diagnosis and saves lives. In contrast, for women over 50 of average risk with average breast density can safely screen with biennial mammography,” Patt said.
She emphasized the importance of discussing screening and different screening strategies with a clinician.
“Cancer screening is part of good health maintenance. Similar to eating healthy food and exercising, cancer screening is a way to reduce your risk of suffering chronic disease and keeping your body healthy,” Patt explained to MNT.
“Women with dense breasts (BI RADS C or D breasts) can benefit from an augmented screening strategy and if they choose not to do that, likely diagnoses will be delayed. And lastly, women should always discuss screening strategies with their doctor. Women with a strong family history of cancer or other factors may have a heightened lifetime risk and require an augmented screening protocol,” she added.
“Cancer screening saves lives. Every time there is an article to heighten awareness of breast cancer screening, women are reminded of the importance of screening, they get screened, they are diagnosed earlier, and their lives are saved.”
— Debra Patt, MD, PhD, MBA
Team Health Accessible
Health & Wellness Editorial Team
HealthAccessible editorial team delivers trusted, accessible, and evidence-based health information for everyone.